I am now a Duke fan — and it’s my neurosurgeon’s fault.
Here’s what happened.
I grew up rooting for Carolina — where my mother and brother went. When it was my turn for college, I went to Wake Forest, but I was in Chapel Hill every weekend. I love the Tar Heels.
I became a social worker and worked with Child Protective Services in Charlotte for 15 years, then I worked for an organization serving foster children.
But then I started having medical issues that made driving to different houses impossible.
In January 2024, my legs gradually stopped working.
I had spine surgery – not with my neurosurgeon hero I’ll introduce soon – to try to fix things. But a few weeks after surgery, things got way worse.
Before all this, I was a jogger. I’d go out, put my headphones on, turn them up all the way, tune out reality, and I’d be in complete bliss.
Now my legs didn’t work at all. Every time I tried to move, walk, or do anything really, I’d fall down — it was like my legs weren’t getting the signal from my brain telling them to move.
Advanced spine, back and neck care awaits
Then I started having trouble using my hands.
I was 53 years old, and my 83-year-old mother had to come live with me. I have a teenage son too. At night they would go upstairs to their bedrooms and I’d be downstairs sleeping on a hospital bed. It was a feeling of hopelessness and isolation — if anything happened, I was on my own.
I couldn’t even go to the bathroom by myself — my mom had to help me clean up. And my son had to see me like that. It was utter debasement.
I wasn’t in pain, but I wasn’t functioning. I went to several surgeons. They had no explanations. They looked at MRIs and said, “There’s nothing that can be done further for you.” One doctor even told me to be grateful for the function I had. I did not appreciate that.
Every time I fell, my mom had to call the fire department to help me up. They came 37 times. Then I was put in the hospital for two and a half weeks. Nothing got better. I got home and fell the next day.
After that, I went to a rehab facility where I went through physical therapy. The physical therapist explained that I hadn’t lost my sensory nerves — that’s why I could still feel things. But I had lost my motor nerves, which is why I couldn’t balance or use my hands or feet properly.
I tried to do the exercises, but I just kept falling.
Eventually I was discharged from the rehab facility. I wasn’t better. I felt like I had lost so much respect in my son’s eyes — and I had, to be honest.
My son, John, is my whole heart. As a father, you have responsibilities to your children. I had reached a point where I was not able to do those responsibilities.
He’s 13, and I thought, I can’t raise him like this. Enough’s enough. I had 52 good years, and I guess everyone’s life ends at a certain time. I believe in quality of life, not quantity.
Everyone told me, “That’s suicidal thinking” — and maybe it was. But I couldn’t live my life the way I was living, and no one I met with had a plan to help me. My spirits sank to a dangerously low level.
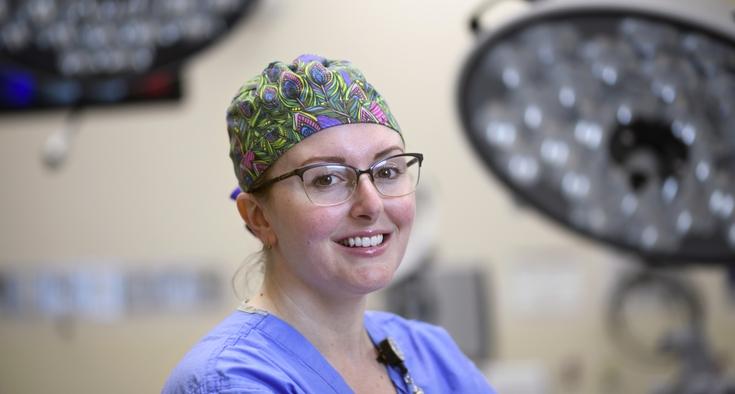
But then I went to see a different surgeon: neurosurgeon Dr. Kelly Ryan Wackerle in Charlotte.
I went in — in a wheelchair — on a Wednesday. She saw the same MRI that everyone else saw — and her response was: You need surgery, badly, and I believe surgery can help you. She arranged everything so I could have surgery the following Monday. She didn’t promise me that I’d be able to walk again, but said she was “optimistic” based on my age, the length of time I had been dealing with this, and my motivation to participate in the rehab I would need.
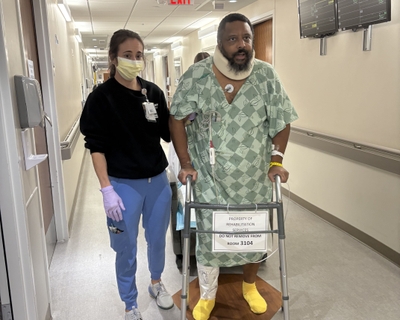
I was not optimistic. But the day after the September 2025 surgery, I walked 20 feet with a walker.
I couldn’t believe it.
Then I went back to rehab. This time, physical therapy was much more meaningful because my legs worked. This time, things got better.
After rehab, I walked into Dr. Wackerle’s office using the walker. All the support staff were happily stunned. They came out and said, “‘OMG! Just look at you! You’re able to walk!’ ‘You don’t know how bad you were before — we don’t know if you remember!’” That was a really special moment.
I told Dr. Wackerle, “I don’t think you quite grasp what you’ve done — but you saved my life.”
I asked her, “What’s the difference between zero and one?” She said “One.”
I said “No — it’s infinite.”
If you have nothing, going from nothing to something is everything.
And that’s what Dr. Wackerle did: She crossed an infinite space. She took a person who had nothing — who had lost the use of two of his legs and was getting ready to lose use of his arms — and she made something.
That’s something I will be grateful for for the rest of my life.
Now I’m in physical therapy. I don’t need a wheelchair, and I’m doing so well that I sometimes forget to use the walker. My mom said if I keep progressing like this, she’ll go back home in March or April.
Now I’m able to do things with my son again — he has his dad back, and you can see a different look in his eyes. His behavior has calmed down at school. He comes home with all these stories he wants to tell me, and he can give me a big hug again.
I was in the hospital for weeks of his school. It was rough. But now he’s being reined back in — we’re going over school work again, I’m reminding him about pleases and thank yous, and I’m making sure he’s doing his chores. We’re coming out of crisis mode.
Just the other day we were picking out what high school he’s going to go to next year. That wouldn’t have happened before. There’s a lot of things that wouldn’t have happened.
Dr. Wackerle looked at the same MRIs as all the other doctors did — but she picked out what needed to be done, she figured out how to do it, and she did it. She did all 15 years of her education and training at Duke.
So now, I root for Duke.
If I could give a message to myself the day I walked into Dr. Wackerle’s office for the first time, I’d say: John, relax — this segment of your life is ending. You’ve made it to the finish line of the very hard part. You survived long enough to get to here, and things get better from here going forward.
Now I have nothing but hope for the future.
*As told to Sarah Bonnema
'We're all here to help people.'
Neurosurgeon Dr. Kelly Wackerle of Novant Health Spine Specialists - Randolph Road performed a posterior cervical decompression and fusion surgery on patient John Taylor (story above).
Some spinal patients come to Wackerle
after an injury caused by sudden force, like a car accident.

Wackerle compares it to a bedsore: “If
you're pushing on the skin for a long time, you're not going to necessarily
feel a lot of pain but you're going to form a bruise. Over time, that turns to
tissue breakdown and worsening.” Similarly, “even a little bit of sustained
pressure on the spinal cord can be damaging.”
The pressure on Taylor’s spinal cord
had caused “what was essentially such a bad bruise of the spine” that it
compromised his spinal functioning below the mid-cervical spine, leading to cervical
myelopathy.
His first surgery, performed by
another surgeon, approached John’s problem conservatively, but “wasn’t enough”
to fix the problem. “Sometimes surgeons hope that ‘less is more,’ but
sometimes, ‘less is just less,’” Wackerle said.
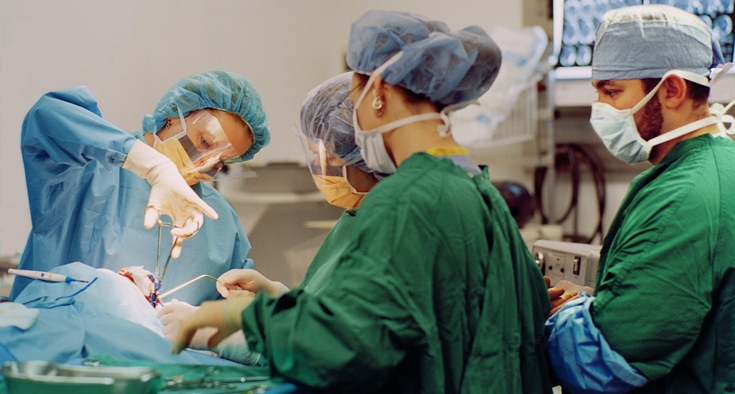
So Wackerle performed additional
surgery: First, she decompressed the area around the spinal cord to relieve the pressure on the spinal cord,
then used rods and screws to keep the bones around the spine in an improved
position. The operation took about 4 hours.
After surgery, “He had a burst of
initial improvement, which is already life-changing,” Wackerle said. “But
what’s exciting for me is that with the coming months, he may see subtle
improvement still.” These gains will come from participating in physical therapy,
doing his physical therapy homework, and following post-surgical restrictions.
Improvements will also come from his
spirit and determination: “A lot of human nature and human recovery depends on
a person's outlook, hope, ability to get up each day and keep trying,” Wackerle
said.
Taylor is just one of many patients
whose lives Wackerle has transformed. (Here’s another patient's story.) The before-and-after stories witnessed by support staff
encouraged team member Kristy Dickens to share this emoji-filled message with Wackerle on a
bulletin board in the office.
"SHOUT OUT TO DR. WACKERLE ON HER SURGERIES. ALL HER POST-OP PATIENTS WHO COME IN, YOU WOULD NEVER KNOW THEY HAD SURGERY UNLESS YOU LOOK AT APPT. NOTES!!!! AND PATIENT FEEDBACK COMMENTS ARE ALWAYS GOOD ABOUT THEIR SURGERIES!!!"
Wackerle said the success is shared by
the whole team: “It doesn’t require a neuro exam or post-op imaging to see
patients go from one function, mood, or degree of pain before surgery to an
improvement after surgery — we can all sense it.”
“We’re all here to help people, and whether someone’s answering the phone, taking vitals, or is the surgeon themselves, we're all part of that same mission of improving lives.”
And, Wackerle adds, she’s always happy
to bring another Duke fan into the fold.