A cancer diagnosis doesn’t have to be devastating. That’s because there has been huge progress in treating the condition that roughly 2 million people in the United States were diagnosed with this year.
Research, therapies and surgery have all come a long way. And patient navigators play a big role in helping those who have received a cancer diagnosis understand every step of the journey.
Think of them as part nurse, part guide, part problem-solver. Nurse navigators are like reliable GPS, specially trained to support patients and their families through what can be an overwhelming experience. They understand the complexities of cancer treatment and help patients coordinate all aspects of their care.
Navigators are not only experts at explaining cancer diagnoses and treatment options, but as registered nurses they are also reliable providers of emotional support.
Thirteen of them serve patients at the Novant Health Zimmer Cancer Institute, part of Novant Health New Hanover Regional Medical Center in Wilmington. They specialize in blood, brain, breast, gastrointestinal, gynecologic, head and neck, lung, prostate and urologic cancers.

As an oncology nurse navigator, Heidi Drueppel focuses on lung cancer, the leading cause of cancer death in the United States.
“When people think of cancer, they often think of what it was 20 years ago: not as many treatment options, people not able to fight it as easily,” Drueppel said. “But we’ve come so far with treatment, and that’s an important part of the patient conversation.”
Here, she explains how nurse navigators develop that relationship with patients and their caregivers.
Supportive care throughout your cancer journey.
What’s the best way to understand your role as an oncology nurse navigator?
I guide patients through their cancer journey by coordinating their care and helping them understand their diagnosis. We are often the patient’s first contact because we call and talk with them before they have established with an oncologist. During that first phone call, we discuss what is needed for their workup. I then order and schedule those tests, assist with managing any symptoms, and help the patient access any resources they need. I am their contact until their oncology appointment and/or lung clinic.
How difficult are those conversations with patients?
Patients are usually diagnosed by a pulmonologist (lung specialist) before being referred to me, but that’s not always the case. There are times that I review biopsy results with the patient and inform them of a cancer diagnosis. It can be an emotional conversation. But we also discuss the positives, which are the many different curable options.
Is cancer generally found during a screening?
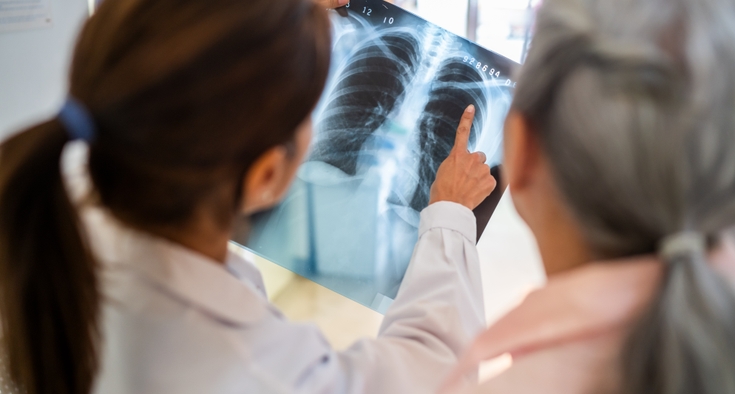
There are numerous ways that we find lung cancer. Pulmonary nodules and/or masses can be detected through a low-dose lung screening. Sometimes they are found incidentally; for example, during a chest CT scan taken after a patient is injured in a car accident or a fall. A patient could also have a symptom such as a chronic cough, and nodules are sometimes noted during a chest X-ray. Of course, being a long-term smoker is the highest risk for lung cancer. Screening is recommended for current smokers and former smokers who have quit within the past 15 years, who are ages 50 to 80 and who have a 20 pack-year smoking history.
What does your day look like when you’re helping someone who is newly diagnosed with cancer?
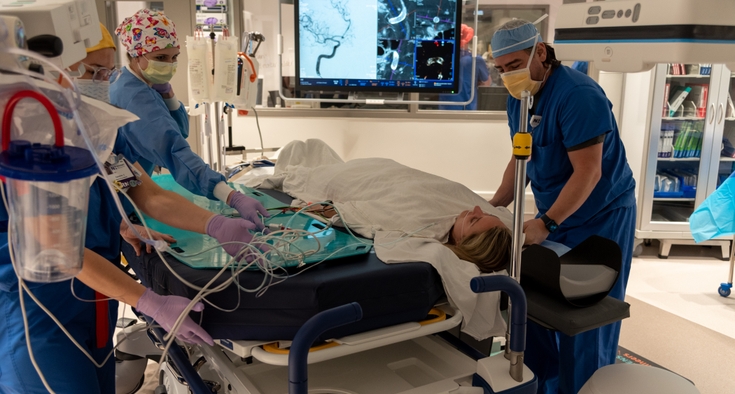
Once a week, I coordinate a tumor board to review cancer cases. The board is a group of lung specialists who discuss cases and reach consensus on a patient’s treatment options and any further work up needed. Our tumor board includes a medical oncologist, radiation oncologist, surgeon, radiologist and pathologist. We meet every Wednesday morning at 7 a.m., and together we look at a patient’s history, imaging and biopsy results. We then see the patients at clinic at 8 a.m., where the doctors meet with patients and their families one-on-one to go over the options. It’s helpful for patients to be seen in the multidisciplinary clinic so they don’t have to go to so many appointments. I am then able to make sure they understand what the doctors discussed and what the next steps are before they leave.
I like to explain everything several times because there’s a lot to remember. The patient, of course, has their oncology team, but I’m always a resource for them, too. What they’re going through can be scary. I’ve worked with cancer patients as young as their late 30s; they’re of all ages and different stages.
When did you know this was the role for you?
Prior to becoming an oncology nurse navigator, I worked in healthcare administration and was an emergency department nurse. I came to the cancer center five and a half years ago as an infusion nurse, administering chemotherapy treatments to patients. I later became the infusion coordinator for the chemo center. I remember observing how one of our breast cancer navigators approached, talked to and helped patients. You’re responsible for giving them vital information and helping them through a very hard time in their life. A closeness develops between you and the patient, and it is rewarding to know that I have the opportunity to help someone.