In his 50s, Reginald Reaves started a regular exercise program. The Greensboro resident had plenty of reasons to take care of himself — his wife, Francine; daughter Alicia; and niece Natasha, whom he considered a second daughter. He had held a variety of jobs over the years, including truck driver and city bus driver, and hoped to work well into his 60s and even beyond. "Outcome with no income is bad math," he liked to joke.
His rigorous exercise routine kept him in action until one day in 2022, when his chest began to hurt while he did pull-ups at the gym. He had a heart attack. “I was pretty healthy, so this heart attack thing hit me by surprise,” Reaves said.
His second heart attack came a year later. Reaves was carrying a heavy, wrapped window at the manufacturing plant where he worked when he felt a pain in his chest. Then the dizziness started. Someone called 911. Francine was terrified when she heard what had happened. Alicia flew home from Michigan to be with her dad.
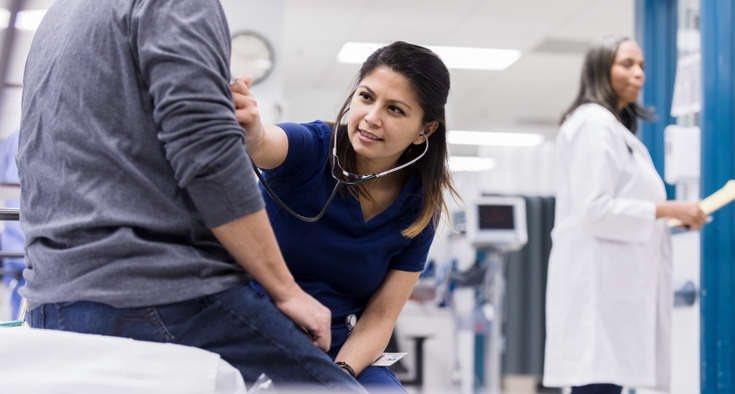
Multidisciplinary care for heart failure.
Novant Heath physicians treated his condition with two stents to improve blood flow and an ICD, or implantable cardioverter defibrillator. An ICD is embedded under the skin and connected to the heart. The device recognizes an abnormal heartbeat and shocks the heart when needed to reestablish a healthy rhythm.

By 2025, those treatments were no longer enough. “Despite medical therapy and interventions to support him and improve his symptoms, his condition continued to deteriorate,” recalled his cardiologist, Dr. Hassan Alhosaini. “He was experiencing significant symptoms of heart failure that affected his ability to perform basic activities of daily living.”
He developed end-stage heart failure, an often-dire condition with a typical survival of six months or less. But Alhosaini, medical director of the advanced heart disease and pulmonary hypertension program at Novant Health’s Heart & Vascular Institute in the Triad, had an idea. If it worked, it could save Reaves’ life.
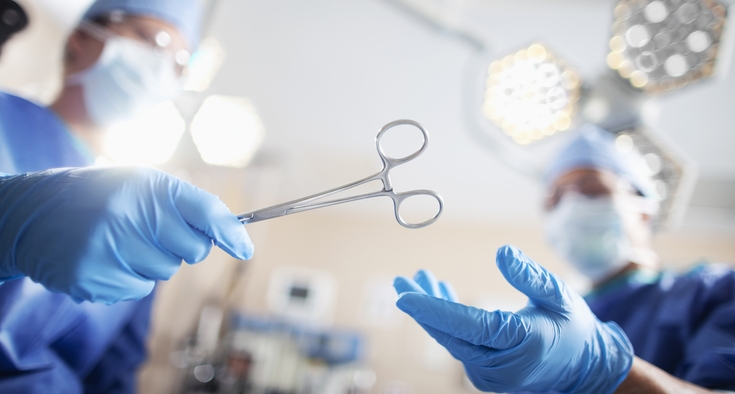
A lifesaving treatment
The only option left was an LVAD, or left ventricular assist device. An LVAD is implanted surgically into the heart to assume the function of the left ventricle.

While the right ventricle of the heart pumps blood to the lungs, the left ventricle is bigger and pumps blood to everything else, including the brain, kidneys and other vital organs. "The vast majority of heart failure in the United States is left-ventricle related," explained Dr. Jesse Madden, a thoracic and cardiovascular surgeon who performs this procedure at Novant Health Forsyth Medical Center in Winston-Salem.
The LVAD was once used as a stopgap measure while the patient waited for a heart transplant. Advances in the last 15 years allowed LVAD therapy to be a lifesaving treatment on its own, Madden said. With this pumping device, Reaves could enjoy his normal activities for five years or more.
There was one more hurdle to cross. Unlike many surgeries, it's not just the patient and surgeon who make the decision to proceed with an LVAD. The patient evaluation includes a surgeon, cardiologist, LVAD coordinator, physician assistant, nurse practitioner, social worker, pharmacist and palliative care provider.
Why such a big team? Because of the care required after surgery. The LVAD is connected to a power source outside the body with a power cord. Patients need to have access to consistent electrical power, including arrangements for emergency power during power outages. The cord requires a clean dressing that must be changed once or twice a week and is difficult to do alone. Close friends or family need to help.
Patients take a blood thinner and other medication. Diet is another issue. "Sometimes when people have heart failure, they don't feel like eating much," Madden said, "but when they get the procedure, they feel so much better that they gain a ton eating with family and friends." Weight management with healthy foods is key.
Reaves assured the team that Francine could assist, and that he would bring the same spirit to his care that he did to his exercise routine. It’s not uncommon for patients with heart failure to be depressed and anxious. But a hopeful Reaves was ready to fight. The delicate procedure was scheduled for October 2025.
An ideal patient
To begin the process of inserting the LVAD, Madden made an incision in Reaves' breastbone as if to perform open heart surgery. He cut a hole in the bottom of Reaves’ left ventricle and sewed the pump there. He stitched the other end of the pump to the aorta. The pump is about the size of a large jar lid.

A heart-lung machine, also known as a cardiopulmonary bypass machine, is available during the multi-hour procedure to take over the function of the heart and lungs as necessary. Typically, though, Madden does not need to stop the heart. Reaves' heart continued to beat on its own. The surgery was a success.
Reaves began outpatient treatment at a rehab facility about a month later. Monitors checked his heart function and blood pressure while he exercised and built back his strength. Some patients consider rehab a chore. “I enjoy going to it,” Reaves said, “because I'm looking for the bigger picture, the better outcome.”
Alhosaini saw him as an ideal patient. “He was very collaborative and definitely has the will to live,” he said. “He's such an incredible guy, bubbly and loving towards his family. Their support was instrumental. He partnered with the team and did everything we asked him to do.”
Reaves has become an informal ambassador for the procedure and has talked with other Novant Health patients considering it. “I live 27 miles away from Novant Health, but I keep going there. That’s how much praise I give them and how much credit I give them for helping me make it through this problem.”
His story shows that heart disease can strike even people who pay attention to their health. "Probably 50% to 70% of coronary artery disease is preventable with taking care of yourself, exercise, eating the right things and taking the meds that your doctor prescribes you," Madden said. "Unfortunately, there's another 30% to 50% that is just bad luck, genetics, or getting older that is really out of our hands, even if you do everything right."
Now 69, Reaves has returned to working part-time as a dishwasher at his niece’s soul food restaurant,
A’Leurer in Greensboro, and he enjoys the camaraderie of the staff. He plans to celebrate his 46th wedding anniversary on Juneteenth with a full heart.