Pain blazed through Alexis Aguiluz’s shoulder that May morning in 2025. It was frighteningly familiar. She had been in great health for the first 20 weeks of her pregnancy, but around week 22, the pain had been the first sign that her liver was bleeding. Though that bleed had resolved after a stay in the hospital, she now suspected it was back. She called an ambulance.
Many Charlotte radio listeners knew Alexis, 35, as an on-air personality with the longtime "Ace & TJ Show," which broadcast until September 2024. Alexis was thrilled about the pregnancy.” She had married Juan, who everyone called J, in October 2023. She couldn’t wait to gather with friends at the baby shower and post photos of her healthy newborn on Instagram.
But when she arrived at Novant Health Presbyterian Medical Center in Charlotte and the obstetrician checked the fetal heartbeat, it was erratic. A few beats, then silence, then a few more beats. Alexis heard the doctor say, “We need to take this little human out right now.” Suddenly the room filled with physicians and nurses. The last thing Alexis remembers is a mask being lowered over her face. She was 25 weeks pregnant.
Baby Benny was born more than three months early. “I was shocked that he could come out at 1 pound, 1 ounce, and still fighting with every ounce of his being, just fighting for his life,” J recalled. “It inspired me to see him.”
Benny would need that fighting spirit to stay alive, along with the skilled nurses in the NICU, or neonatal intensive care unit, at Hemby Children’s Hospital located within Presbyterian Medical Center. A physician warned J that Benny’s chances of survival were slim. The baby was a “micro-preemie” — tiny, weak and ill. J thought: There’s still a chance.
Providing the highest level of car to premature and critically ill newborns
A tiny fighter surrounded by care
Alexis remained intubated and sedated in the ICU as doctors worked to resolve her liver condition. When she awoke three days after Benny’s birth once her condition was stable, she asked if her baby had survived.
A nurse washed and braided Alexis’s hair the morning that Alexis met her son. Everything was shocking to Alexis: the NICU with dozens of struggling babies. The beeps and alarms from the machines. Her own child, about the size of a hand. He looked like an alien, Alexis recalled, with wires sprawling from his body. After the visit, “I had a whole breakdown in the hallway,” Alexis said.
J couldn’t join her that morning because he was working at their food truck, Bodega Food Wagon. He had spent virtually all his time in the hospital after Benny’s birth, either with his son or his wife. He faced the added stress of keeping their business going but sought to remain positive.
They both felt grateful for the big, devoted team looking after Benny. The NICU works on a system of primary nurses who regularly care for a particular infant. The system helps build rapport with parents and allows nurses to intimately know the babies in their care. Benny had eight primary nurses.

Avery Barrow was one of the nurses on the day shift. She quickly became attached to the little boy who was striving to survive. One evening, Benny’s blood pressure dropped towards the end of her shift. She briefed the night nursing team and headed home but couldn’t fall asleep. “I was worried he was going to crash,” she recalled. “But that’s the thing with Benny,” Barrow marveled. “He would throw stuff at us, we’d pivot, and he’d respond.”
For several months, it wasn’t clear if Benny would pull through. His lungs were underdeveloped, he required 10 blood transfusions during his stay, and he needed surgery to repair a hernia.
Alexis was initially afraid to buy him many clothes or finish the nursery, worried she might jinx the outcome. Alexis and J became such familiar figures in the hospital cafeteria that one server began regularly praying for their son. A brewery that had hosted the couple’s food truck surprised them by leading a fundraiser.
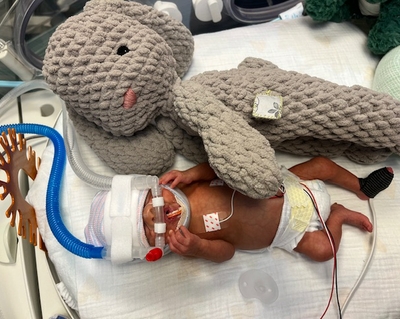
Over time, Benny gained weight. One primary nurse taught Alexis and J how to diaper Benny and take his temperature once he was strong enough to be handled. Another took pride in making sure his clothes were fresh for Alexis and J’s arrival.
Alexis spent long days in the NICIU, absorbing medical terminology and procedures and getting to know the other parents. Her outgoing personality, honed from years on the radio, drove her to learn everyone’s story.
The doctors and nurses began introducing her to new NICU parents to help them get acclimated to their surroundings and understand what to expect. One look at their expressions and Alexis could guess what they were feeling. Strangers became friends, and Alexis still goes out once a week for margaritas with a group of former NICU parents. They’ve “trauma bonded,” as Alexis puts it, through one of the worst times of their lives.

Benny De Los Santos was expected to be born on Sept. 6, 2025. He left the NICU for home on October 20, weighing 6 pounds, 10 ounces. Though still using supplemental oxygen, he has climbed to over 7 pounds.
The couple believes their faith in God, their family and friends, and their team of clinicians carried them through. "The Novant Health staff was amazing," Alexis said. "I mean every person — the doctors, occupational therapy, physical therapy, respiratory support. We had so many people that just were so loving and such good people.”
The NICU team feels the same way about them. “Benny is extremely strong and remarkable,” Barrow, the nurse, said. “And so is the family.”
‘Little miracles every day’
Having a newborn requiring intensive care is one of the most traumatic experiences a parent can face. The NICU team at Hemby Children’s Hospital is here to support, educate and comfort parents while providing round-the-clock, experienced care for infants.
The NICU serves seriously ill newborns from other Novant Health hospitals in outlying cities, along with babies born at hospitals outside the Novant Health system. “They could come to us for blood sugar issues, feeding intolerance or a surgical procedure that they need right away,” explained McKenna Puckett, a NICU nurse and one of Benny De Los Santos’ nighttime nurses.
“It could be they need antibiotics. They could have respiratory distress. They might have swallowed some amniotic fluid in utero or meconium,” a substance typically passed after birth.

Puckett was drawn to NICU work to see babies progress from their first day of intensive care to the moment they leave with their families. She came to love the chance to serve entire families, knowing a baby’s time in the NICU touches parents, siblings and extended family.
“There's a lot more good than bad that happens in the NICU,” Puckett said. “We get to see these tiny babies eventually be strolled out in their stroller and go home with their parents on room air and bottle feeding. We get to see little miracles every day.”