Dr. Jeffrey Everett remembers the moment his career shifted.
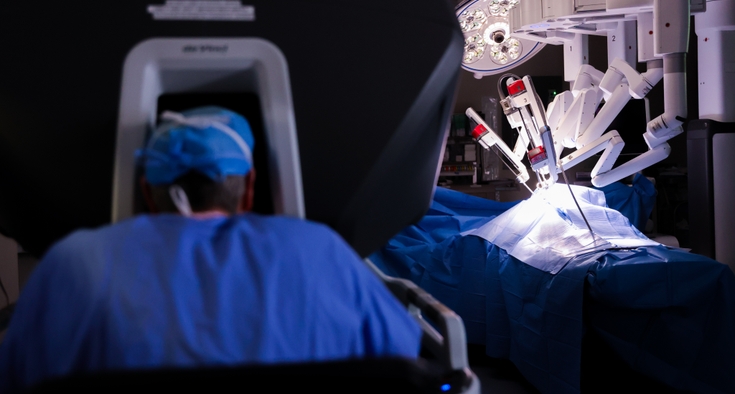
At a surgical conference in the early 2000s, Everett, a cardiothoracic surgeon, sat down at a console connected to a new piece of technology called the da Vinci robot, slipped his fingers into the controls and watched tiny instruments perfectly replicate his movements inside a training model.
“It was like a light switch going off,” he recalled.
For Everett, the robot unlocked a new way of operating. He saw the possibility of repairing or replacing a heart valve with precision through a few small ports rather than a large chest incision.
Everett and a fellow surgeon from the University of Iowa Healthcare system put together a business proposal to persuade their hospital leaders to invest in a da Vinci robot.
Their pitch worked, and Everett became the first surgeon in Iowa to perform robotic surgery — at a time when few hospitals had even begun using surgical robots.
Fast‑forward to today, and Everett is the nationally renowned surgeon leading the Charlotte region’s first dedicated robotic mitral valve program, offering patients smaller incisions, less bleeding and dramatically shorter, less painful recoveries.
Take the first step and find the heart care you deserve
Until Everett arrived in Charlotte earlier this winter, patients in the Carolinas had to travel to the Medical University of South Carolina in Charleston, South Carolina, or East Carolina University in Greenville, North Carolina, to have robotic mitral valve surgery.
His move doesn’t just eliminate those long drives — it marks the beginning of a new chapter for cardiac care in the region, bringing leading-edge surgery closer to home.
Why the mitral valve matters
The mitral valve is a small but crucial gateway between the heart’s left atrium and left ventricle, opening and closing to keep blood moving from the lungs to the body.
It’s also one of the valves that’s most likely to wear out, leading to mitral regurgitation — when the valve fails to close completely causing blood to flow backward — or mitral stenosis, when it narrows and restricts flow.
Some patients learn they have mitral valve disease after a doctor hears a heart murmur; others feel symptoms like fatigue, shortness of breath or an irregular heartbeat. Mitral valve problems can be present at birth or develop later in life due to aging, infections or autoimmune disease.
For years, fixing or replacing the valve meant open‑heart surgery through a full chest incision (called a sternotomy) that involves cutting through the breastbone and spreading the ribcage — an effective approach, but tough on patients.
Less invasive approaches through smaller incisions followed but still forced surgeons to work through tight spaces with limited visibility — “like building a ship in a bottle,” Dr. Everett said.
How robotic mitral valve surgery works
Robotic mitral valve surgery changed that. It lets surgeons repair the valve through tiny ports between the ribs, using 3D visualization and precise robotic instruments controlled by a surgeon from a nearby console.
The operation takes about two hours longer than open surgery; the robotic procedures typically last four to five hours from start to finish, Everett said.
But recovery is dramatically easier. Most patients stay in the hospital for only three nights — some younger, healthier patients leave after just two nights — and go home with small incisions and minimal pain.
By contrast, patients recovering from mitral valve surgery with a sternotomy often stay four to five nights, Everett said, and face three months of lifting restrictions. Even the strongest patients, Everett noted, “go home with pain, and it’s going to be months before they forget that they had that surgery.”
A hands-on path to the heart
Everett grew up on a farm in the northern Ohio town of Deerfield, with plans to become a veterinarian. His father died from heart disease when Everett was young, a loss that moved the family off the farm and steered Everett toward medicine — and eventually the operating room.
The launch of the robotic mitral valve program reflects Novant Health’s commitment to bringing leading-edge care to the communities we serve and expanding access to options that were once only available hours away. Dr. Jeffrey Everett’s arrival is the latest example of how we’re strengthening a heart and vascular program grounded in innovation, safety and the best possible outcomes.
In medical school he quickly realized general surgery wasn’t a fit, but a two‑week rotation in cardiac surgery clicked. He was drawn to how quickly heart surgery can solve a problem compared with procedures that lead to long, drawn-out recoveries.
Cardiac surgery “is not a slow progression — it’s a sudden fix,” Everett said.
He went on to follow the long, traditional path of full general surgery training followed by a cardiothoracic fellowship — and built a career at academic centers, where he taught and helped develop programs.
Novant Health offered him the chance to build the region’s first robotic mitral valve program — and with two of his three adult daughters now living in the Carolinas, the move to Charlotte made sense on a family level, too.
Building a small, highly trained team
Robotic cardiac surgery is a team endeavor, and Everett is meticulous about how he builds his. Bedside assistants, perfusionists (who operate the heart-lung machine), anesthesiologists and nurses all train for robot‑specific roles — from specialized breathing tubes to port placement and instrument exchange.
“We keep the core team small and consistent,” he said.
For months before the first surgery in Charlotte, the team practiced on models, trained with proctors and ran simulations — an approach Everett has used to launch programs at previous institutions.
Everett and his team performed two robotic mitral valve surgeries during the program’s first week serving patients in early March, with several more scheduled shortly after — "a very strong start” for a brand-new program, he said.
Who’s a good candidate for mitral valve surgery?
Everett’s rule of thumb: Patients who need isolated mitral valve repair or replacement —and don’t require multiple other cardiac procedures at the same time — are often good candidates for the robotic surgery.
Contrary to common misconception, robotic mitral valve surgery isn’t an option for the sickest or most fragile patients, because it involves a longer time under anesthesia and on the bypass machine. “I worry about the kidneys, the brain, and how they can handle that increased time,” he said.
And while the robot often gets the spotlight, another misconception persists: that the robot is “doing” the procedure. Everett laughs at that. “I’m operating the entire time,” he said. The name “robot” can mislead people outside medicine. In simple terms, it’s a sophisticated tool under total control of the surgeon.
The da Vinci system gives Everett a 3D view, and his hands move instruments with millimeter precision inside the chest. All the motion is internal; he’s at the console guiding every stitch.
Recovery is faster and smoother with robotic heart surgery, he said, but it’s still heart surgery.
“A lot of people come in and think it’s an outpatient procedure and ask, ‘Am I going to go home later that day?’ I say, ‘No, you will have just had heart surgery,’” Dr. Everett said.
A better experience for patients
The new program gives cardiologists in the region a clear, local referral pathway for patients who need mitral valve repair and could benefit from the robotic option.
And Everett encourages patients to advocate for themselves by asking their cardiologists whether they could be candidates for robotic surgery and requesting a referral to a surgeon with extensive experience who can evaluate their case.
For Everett, the most rewarding days in the operating room are ones when the team moves seamlessly, the repair is strong and the patient sails into a smooth recovery thanks to robotic surgery.
“Most patients are just ecstatic that they had it that way,” he said.