Your heart rarely sends a neatly labeled warning when something isn’t right. A flutter, a twinge of chest pain or a moment of breathlessness can be easy to dismiss — until it isn’t. For the most accurate picture of how well a heart is functioning, cardiologists rely on cardiac imaging. This technology helps detect and diagnose heart problems early, before warning signs turn into emergencies.
Cardiac imaging helps identify the underlying cause of symptoms such as chest pain, shortness of breath and palpitations by giving doctors a detailed view of how the heart is working. It plays a key role in diagnosing major conditions including coronary artery disease, hypertension-related heart changes and rhythm disorders such as atrial fibrillation.

“Cardiac imaging is essential to cardiology as a whole,” said cardiologist Dr. Andrew Milbridge of Novant Health Heart & Vascular Institute in Wilmington. “It can be shocking for patients to learn they have a cardiac problem, but I reassure them that the tests we do are very safe, noninvasive and often can help identify some key red flags to help prevent something serious down the road.”
General cardiologists collaborate closely with interventional cardiologists and cardiac surgeons to deliver comprehensive heart care, from identifying blocked arteries to ensuring healthy blood flow to the heart muscle. Cardiac imaging is essential not only for accurate diagnosis, but also for treatment planning — from medical management to advanced procedures when needed.
Symptoms don’t always mean something is wrong, but they are a reason to check in on your heart. Here, Milbridge explains how cardiac imaging helps cardiologists understand what’s happening in the heart and how it can guide next steps.
Nationally recognized heart and vascular care.
Cardiac imaging is common — and for good reason.
Heart disease is widespread, and early diagnosis can make a real difference. That’s why cardiac imaging is used so often.
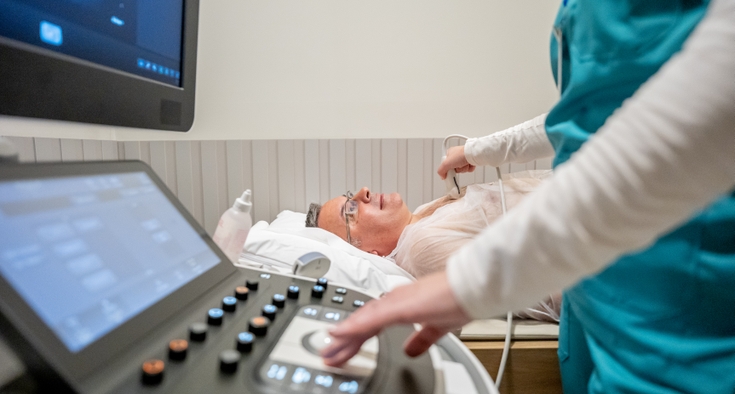
The most common test is echocardiography, a noninvasive ultrasound that uses sound waves to create real-time images of the heart. This is similar to the technology used during pregnancy ultrasounds.
An echocardiogram allows cardiologists to assess heart muscle strength and valve function and is often the first step in determining whether further testing is needed.
The ‘best’ imaging test depends on your symptoms.
Not every patient needs the same type of imaging. Cardiologists select tests based on individual symptoms and risk factors:
- Coronary CT scans (coronary computed tomography angiography, or CCTA) provide a noninvasive view of the heart’s arteries to see if plaque buildup is significant enough to contribute to symptoms like chest pain or shortness of breath.
- Coronary artery calcium scoring measures calcium buildup in the arteries. While lower resolution than CCTA, it helps assess risk and guide preventive care, such as starting cholesterol medication or low-dose aspirin in younger patients with a strong family history of heart disease.
- Nuclear stress testing uses a small, safe amount of radioactive tracer to track blood flow to the heart during rest and stress. This helps identify blocked arteries, areas of heart muscle damage, and a patient’s risk for heart attack, guiding further testing or treatment.
- Cardiac MRI uses magnets and radio waves to produce highly detailed images of the heart from multiple angles, without radiation. It allows cardiologists to assess heart function, tissue health, scarring, inflammation, congenital abnormalities and certain cardiomyopathies (conditions that make it hard for the heart to pump blood). Because the test takes longer and is more costly, it’s usually reserved for later in the diagnostic process or when highly detailed information is needed.
Cardiac imaging guides treatment decisions before invasive testing.
Imaging plays a crucial role in evaluating symptoms and detecting structural heart problems, allowing many conditions to be managed with medication and lifestyle changes. Doctors typically turn to invasive procedures only in emergencies or when symptoms persist despite treatment, using imaging to ensure those steps are truly necessary.
Cardiac imaging supports proactive, personalized heart care.
Doctors can see issues like narrowed heart valves or clogged blood vessels sooner and keep an eye on them over time, which often means treating them with medicine, healthier habits or simpler procedures.
Catching problems early can sometimes prevent the need for more aggressive tests or treatments later. By starting with noninvasive imaging such as echocardiograms, CT scans, nuclear stress tests or MRIs, cardiologists can track changes over time and tailor care to each patient — intervening only when it’s truly necessary.