Elaine Smith doesn’t take big decisions lightly — especially when they involve medical care. So when her husband, Bill Loche, learned he needed major heart surgery, the retired nurse did what came naturally: She dug into the data, asked tough questions and made sure the care team they chose felt right, on paper and in person.
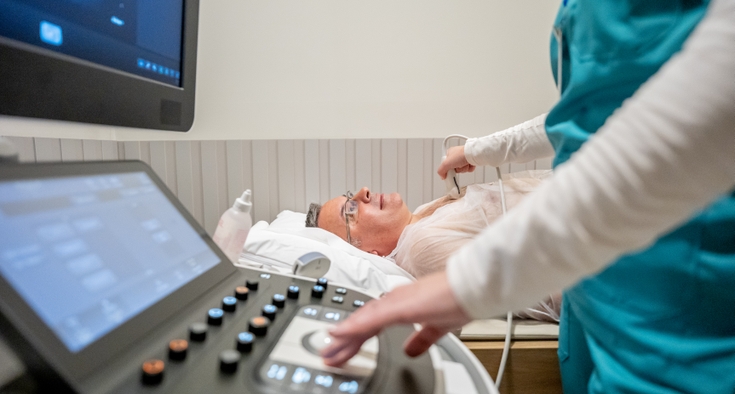
When Loche, 71, went for an annual visit with his cardiologist in July 2025, he mentioned some pain in his left calf. A prior ultrasound showed blockage in one of the arteries in his leg. Given this information, Loche asked if he should have his coronary arteries checked. His cardiologist agreed and scheduled a diagnostic CT scan (a detailed 3D X-ray of the heart) and cardiac catheterization (a test where a doctor threads a thin tube through a blood vessel to the heart to check blood flow and look for blockages).

The diagnostics showed that Loche had a 95% blockage in three coronary arteries, which supply blood to the heart muscle. His cardiologist recommended surgery and referred him to Dr. Peter Kane of Novant Health Heart & Vascular Institute - Wilmington, who specializes in thoracic, cardiovascular and vascular surgeries.
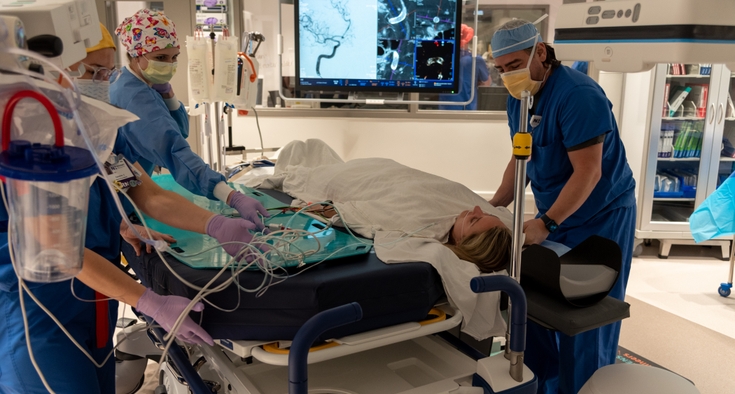
Loche, a retired engineer and avid golfer, learned he would need coronary artery bypass graft (CABG) surgery. More commonly referred to as simply bypass surgery, it improves blood flow to the heart. During the procedure, a surgeon takes a healthy blood vessel from another part of the body — often the chest, leg or arm — and uses it to create a new pathway around a blocked or narrowed coronary artery. This “bypass” allows oxygen-rich blood to flow to the heart muscle again.
Bypass surgery is a common procedure — Kane said vascular surgeons at New Hanover Regional Medical Center perform around 350 of them a year — but that doesn’t mean it’s not serious. Loche would have an open-heart procedure requiring weeks of recovery, followed by cardiac rehabilitation, a program that focuses on holistic heart health improvements through lifestyle changes like exercise, stress management and nutrition.
This is why Smith, who worked in healthcare for 45 years, went into research mode. The Leland, North Carolina, resident was interested to learn how the cardiac program at nearby Novant Health New Hanover Regional Medical Center, just across the river in Wilmington, stacked up against the programs at other well-known North Carolina hospitals.
Guidance and expertise to keep your heart strong and healthy.
Confidence in their care
Smith reviewed Kane’s profile online, scrutinizing his education, experience and patient reviews. Then she did a deeper dive into the cardiovascular program statistics, looking at publicly available data on cardiothoracic surgical outcomes.
From her last career as a dean of the College of Nursing and Public Health at Adelphi University in New York, she recalled a national database of statistics on cardiovascular surgery programs. She searched online and found the Society of Thoracic Surgeons, or STS, national database, which allowed her to compare programs against each other. She liked what she saw, but the statistics were only part of the equation.
“We spent quite a bit of time with Dr. Kane,” she said. “He answered Bill’s questions about the procedure and was extremely gracious about explaining his quality outcomes to me, as well.”
The couple felt confident with what they heard from Kane, although Bill was skeptical about something the surgeon told him.
“Dr. Kane said, ‘You’re active now, but you’re going to have more energy after surgery,” he recalled. “And I thought, ‘Yeah, yeah, yeah.’ I didn't quite believe it. I figured I was getting tired because I was getting older.”

Dr. Peter Kane has earned national recognition for excellence in cardiothoracic surgery, landing on Newsweek’s prestigious list of America’s Leading Doctors 2025.
Among 185 surgeons nationwide selected for the honor, Kane ranked No. 12 overall — the highest-ranked cardiothoracic surgeon in North Carolina — and was one of only nine physicians in the state to make the list. The recognition highlights his high-performance outcomes in coronary artery bypass graft surgery, a cornerstone of advanced heart care.
The couple’s decision to stay close to home for bypass surgery came down to cold facts and a warm feeling.
“Comparing those statistics, coupled with seeing how Dr. Kane and Bill connected, I felt comfortable that we’d be safe sticking with our regional medical center,” Smith said. “It’s a huge decision, and you want to make the best choice.”
On a fast track to healing
Kane scheduled surgery quickly – the week after the initial consultation.
That was a relief to Loche, who didn’t want to wait. “That was a blessing,” he said. “It didn’t give me too much time to think, and I am one to overthink things. I knew enough to be comfortable about surgery. When the time came, I was ready.”
He spent a week in the hospital, including three days in the intensive care unit. He called the care he received in the ICU “fantastic” and said the step-down unit was, as well.
“If I hit the button — whether I was in pain or needed to walk to the bathroom, someone answered within 15 seconds to assess the situation. If it was urgent, they came in right away,” he said.
How quickly the recovery process goes is largely up to the patient, Kane said. Those who follow recovery and rehab recommendations can return to their normal activities sooner than those who don’t.
Loche, who describes himself as restless, was eager to get back to his old life. But before beginning rehab, he needed to take it easy. Kane had prepared them for what recovery might look like. Loche spent a lot of time in a recliner but could still walk around the house and eventually around the block.
During the first several weeks, nurses visited him at home twice a week to monitor his progress, see how the surgical incisions were healing and answer questions. They tracked his weight and ensured he was getting enough calories and nutrition to heal well.
Kane had advised that around the four-week mark, they’d likely see a significant change in how Loche was feeling, and that’s when both Loche and his wife noticed a change. Friends who visited regularly commented on how much better he looked at week four, too.
“I thanked them for lying about how I looked earlier,” Loche quipped.
High praise from a tough critic
Kane had told Loche there was a chance, as a result of surgery, he could develop atrial fibrillation (AFib), an irregular and often rapid heart rhythm (arrhythmia) that can result in poor blood flow and increased stroke risk. Loche experienced its symptoms two weeks post-surgery.
He went to the ER and was “seen promptly,” he said. “As I was being brought down the hallway into a room, the ED doc, Dr. Alex Snyder, was waiting for me,” he said. “The care and attention I got were phenomenal.”
As a result of AFib, he had three heart medications added to his regimen. He’s already down to one additional medication, and that will be removed soon. He goes to cardiac rehab three days a week, where he’s monitored while doing a series of exercises.
Even Smith, the self-described “tough critic,” gives the facility and team high marks.
“Novant’s cardiac rehab is a very, very impressive facility,” she said. “They have an amazing team with exercise physiologists, registered nurses and dietitians, stress management consultants. The interactions Bill had there — and the monitoring and educational components were top-notch. They have a great program that includes lectures that families and friends can attend.”
Seeing the cardiac rehab center was a full-circle moment for Smith, who had worked as a nurse in one such unit when she was just 24 years old. The concept was just emerging at the time.
The future is bright
Smith, who stays active by swimming and walking, has been elevating her culinary skills in retirement. “That’s come in handy now,” she said. “I’m getting creative with heart-healthy recipes, which is beneficial to both of us.”
So is the exercise Loche has begun to get back into. He’s chipping and putting now and plans to start swinging a club in January to be back on the golf course in February. As for Kane’s promise that he would have more energy? “He was right,” Loche said. “I do have more energy now. I can keep up with Elaine when we’re walking.”
Loche calls the support he’s received from his daughter, family, friends, his medical team and his golf buddies “phenomenal.”
“We all had our roles to play to get us to where we are now,” Smith added. “The wonderful care team was a big part of it, and it’s been gratifying to see how well it all worked. We’re extraordinarily grateful for the excellent outcomes.”