What would it be like to take your son to a routine doctor’s appointment — for swimmer’s ear, of all things — only to learn that your daughter who happened to tag along has a life-threatening medical condition?
The Smith family of Wesley Chapel, North Carolina, near Charlotte, can tell you. And they don’t think anything about that appointment was coincidental.
This is a story about a doctor who noticed something was amiss and instantly responded. Her observation triggered a chain reaction that provided life-saving care.
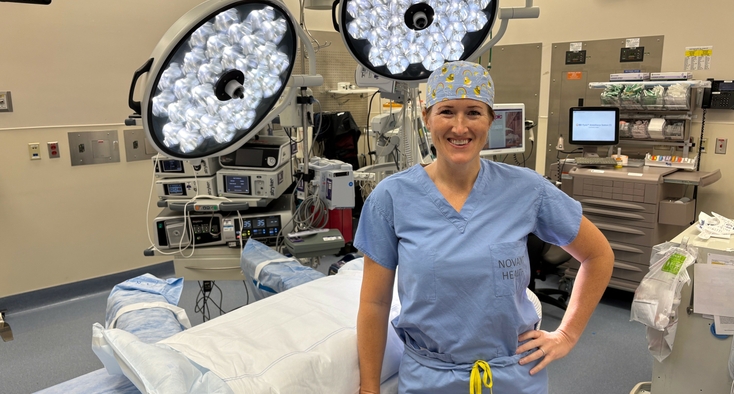
Here’s their journey, with notes from the doctors who helped: Pediatrician Dr. Pamela Young of Novant Health Matthews Children’s Clinic and pediatric hematologist-oncologist Dr. Christine Bolen of the St. Jude Affiliate Clinic at Novant Health Hemby Children’s Hospital.
Allison Smith: I can still see it all play out in my mind. Our 10-year-old son Wilson had been saying his ears hurt. When you’ve got seven kids, you’ve got an ear-checker. I looked and knew it was swimmer’s ear.
It happened that Dr. Young was working. She’s been our family’s pediatrician since our oldest was born in 2008 and we’ve loved her all these years. I grabbed the appointment, thinking we just needed a prescription for ear drops.
Before they left, our then-6-year-old Annie asked, “Can I go with Dad and Wilson to Wilson’s appointment?” This was out of character for her, because she’s usually a homebody, but we said “Sure, why not?”
We wouldn’t be where we are today if Dr. Young hadn’t been the pediatrician that she is.

Dr. Pamela Young: I’ve been a pediatrician since 1993. One of the biggest challenges in all of medicine is not to become complacent. You have to continue to be a questioner and a learner. You have to remain curious.
I often remind myself: “It's a busy flu season, but just remember that not everybody who has a fever today has the flu.” I try to look at each patient individually and pay attention to detail.
Annie sat quietly through Wilson’s appointment. Right as they were leaving, her shorts rode up and I saw the edge of a giant bruise. I asked how it happened, and her dad said she had run into a wall charger. But the bruise was much bigger than I thought it should have been.
In the moment, I didn’t ask myself, “Should I look into this or not?” Sometimes it’s a gut instinct, like, “This just isn't right.”
So I examined Annie, and saw a couple more bruises that didn’t have a reason for being there. That’s when I said, “I think we need to look into this.”
I ran a blood test in our office. When I saw the results a few minutes later, I immediately called Christine Bolen.
Expert treatment for pediatric cancer and blood disorders.

Dr. Christine Bolen: Dr. Young is a very experienced, respected pediatrician, so when she expressed concern regarding the bruising, I knew it was a true concern even without the labs.
Then she reviewed the lab results with me.
Platelets are cells in your body that help you form a blood clot and prevent you from having ongoing bleeding. A normal platelet count is 150,000 to 400,000 platelets per microliter of blood.
Annie’s platelet count was 3,000.
She was also anemic, meaning that her healthy red blood cells were low.
When I see platelet and red blood cell counts as significantly low as Annie’s was, my first concern is acute leukemia — the most common form of childhood cancer.

Allison Smith: My husband, Jason, texted me, saying that Wilson did have swimmer’s ear, and they were doing some blood work on Annie. I didn’t think much of it. Then he called and asked, “Are you all by yourself?”
I was with my mom, aunt, and the kids, so I walked back to the woods behind our house to be alone.
Then Jason said, “We need to get Annie to Hemby Children’s Hospital. Dr. Young thinks she may have leukemia.”
I just fell to my knees.
My mom found me and asked, “What’s wrong, Allison?”
I don’t know that I even said anything back. I was there, but I wasn’t there — my mind was racing all over the place. I went into the house and just started grabbing random things to pack.
My mom and kids kept asking, “What’s wrong? What’s going on?” I realized I needed to answer, so I said, “They think Annie has leukemia.” And then I started bawling.
My mom hugged me. Eli, our 14-year-old, was like, “I'll pack stuff for Dad.” Maggie, our 13-year-old, went and got a couple of Annie’s favorite stuffed animals and some gowns.
I remember thinking, “I can't leave with the kids seeing me like this.” They had never seen me this upset.
So I pulled them together and said, “Hey guys, listen — during our nightly Bible reading, we’ve talked about how sometimes God puts us in valleys and we don’t know why. Right now we're fixing to go into a valley. I don't know why or what all this is going to look like.
“But we do know that we're going to get on the other side of the valley, on top of the mountain again. Right now I'm a little scared and I don’t know what's going on, but I need y’all to know that everything’s going to be okay. God knew we were going to be in this before we even did, and He’s not going to let us go alone.”
Then I left to go join Annie.
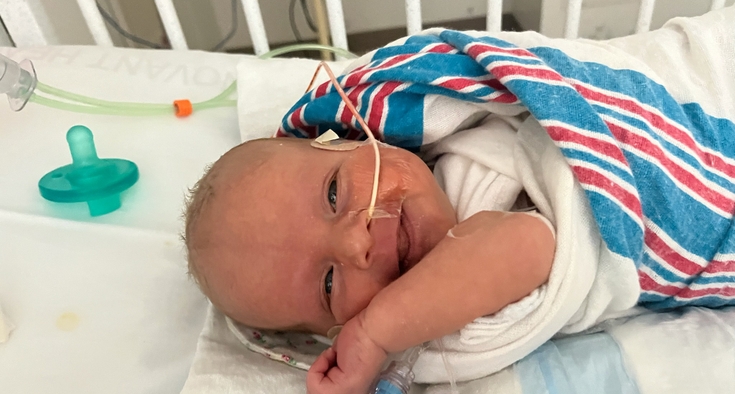
Dr. Christine Bolen: We immediately admitted Annie to Hemby Children’s Hospital.
Our first goal was to improve her blood counts so they were at a safer level, which we accomplished through transfusion. Then we needed to understand why they were so low.
After a few days of further evaluation, we ruled out leukemia.
Her parents were highly relieved, which I get. But I was actually more worried, because now we were looking at a life-threatening condition called aplastic anemia.
Aplastic anemia is an abnormal immune response where your own immune system attacks the cells that produce and grow healthy blood cells. Although it’s not cancer, in some regards it’s more concerning than cancer.
In aplastic anemia, your bone marrow — the “factory” that makes your blood cells — isn’t making platelets, white blood cells, or red blood cells at a normal level.
White blood cells fight infection, and so having very low numbers increases your risk for serious infection. Fungal infections, in particular, can be lethal if you don’t have sufficient white blood cells.
Aplastic anemia is rare. I see several patients a month with acute leukemia, but only two to three patients per year with aplastic anemia.
But Novant Health has a relationship with St. Jude Children’s Research Hospital. Within four days of Annie’s diagnosis, I was able to present her case to St. Jude Children's Research Hospital’s expert bone marrow failure team. This team is composed of individuals whose entire careers are dedicated to treating rare bone marrow failure syndromes like aplastic anemia.
They agreed that the best treatment option was to pursue a bone marrow transplant at St. Jude Children’s Research Hospital 500 miles away in Memphis — ideally, within the next eight weeks.
In the meantime, Annie required ongoing blood transfusions and needed to be monitored closely for signs of infection. Plus, we had to find a match for her bone marrow transplant. Thankfully, all of this could be done here in Charlotte at the St. Jude Affiliate Clinic at Novant Health Hemby Children’s Hospital.

Allison Smith: We’ve had several people say, “How’d y’all get to St. Jude?” I said, “God sent us here.” We never even contacted St. Jude.
Dr. Young got the ball rolling by sending us to Dr. Bolen and the St. Jude Affiliate Clinic at Hemby Children’s Hospital — and once the ball was rolling, we got on the ride and went with it.
Dr. Christine Bolen: Usually, the best donor for a bone marrow transplant is a full sibling.
And when you have six siblings, the odds become 80% that you’ll find a match from one of them.
Allison Smith: My husband said that God blessed us with six other kids for a reason. He knew we would need one of them. On one level, this was a bit of family humor. But for us it also ran deeper.
Not one of our kids ever questioned having to get tested to see if they were a match for their sister. They were rock stars.
It came back that two of the boys were a match. When Annie told them, “We have two winners: The first winner is Wilson, and the second winner is Eli,” all the kids were cheering and jumping up and down. You would have thought they just won $100 or some special contest or something.”
The team at St. Jude decided Eli, age 14, would be the donor.
While we waited for her transplant, we visited the St. Jude Affiliate Clinic here in Charlotte two to three times a week for blood work, blood and platelet blood transfusions, and monitoring.
They made us feel like family from the beginning. When she came in, they’d call her by name.
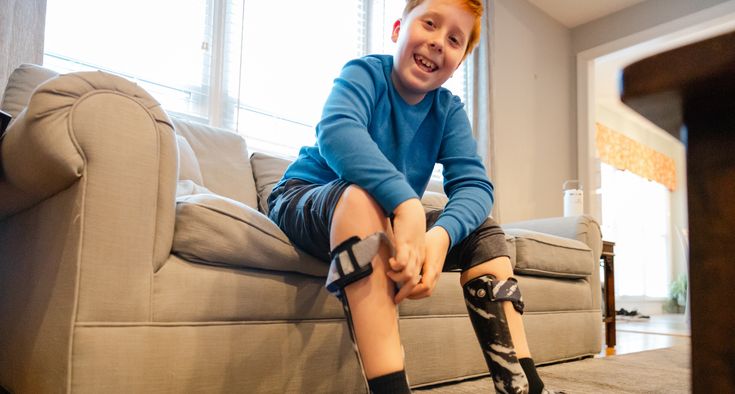
Eventually, Annie had to get a central line put in at Hemby Children’s Hospital. We dreaded it. It was another terrible reminder: “This is really real.” But Annie handled it like a champ.
When we left for Tennessee at the end of September for her transplant, her Hemby nurses had a sweet note and a horse LEGO set for her to take along. They knew she loved horses.

Dr. Christine Bolen: In a month, Annie went from diagnosis to transplant. It was the fastest I’ve ever seen, which was in her best interest, because prompt diagnosis and transplant reduces the risk of contracting a life-threatening infection.
Now Annie’s had a successful bone marrow transplant, and she’s recovering well without any unexpected toxicities or infections.
She’s still considered immunocompromised, so even though her prognosis is good, she needs to be very guarded with respect to possible exposure to infection. Most children can’t go back to school for a year. Thankfully, Annie’s family already home-schooled.
Now that she’s back home, she’ll alternate visits every few weeks between seeing us here in Charlotte at the Affiliate Clinic and returning to Memphis. As she recovers and her immune system develops, more of her care will be here at the Affiliate Clinic than St. Jude.
Annie was incredibly brave throughout this. When we asked her to do hard things, she did hard things — and so did her siblings and her family. They rose to the adversity.

Allison Smith: Annie came out with her own story seven years ago when I almost died giving birth to her. But God's like, I still have more story for this little girl.
Through all this she's never fussed and said “No, I can't do that.” She's always looked straight ahead and said, “I’ll do it.”
I am so grateful that my pediatrician was on top of it.
Dr. Young noticed Annie, and it wasn't even Annie's appointment — it was for her brother. But she saw Annie, and because of her care, we’re here. And because she knew what to do next, we went right into the care she needed at the Affiliate Clinic and then St. Jude.
Words can’t express how thankful we are for Dr. Young and the physician she is.
Dr. Young: I take the responsibility of my patients’ health very seriously and try to bring my best each day. I am so thankful that on that I day I trusted my intuition that something was not right and that additional investigation was warranted.

If you’re between the ages of 18 and 35 years old, Dr. Christine Bolen encourages you to consider joining the National Marrow Donor Program. A simple cheek swab could potentially save a life — just as Annie’s brother Eli saved hers.